Type 2 Diabetes Symptoms Causes and Treatment Explained
What is Type 2 diabetes
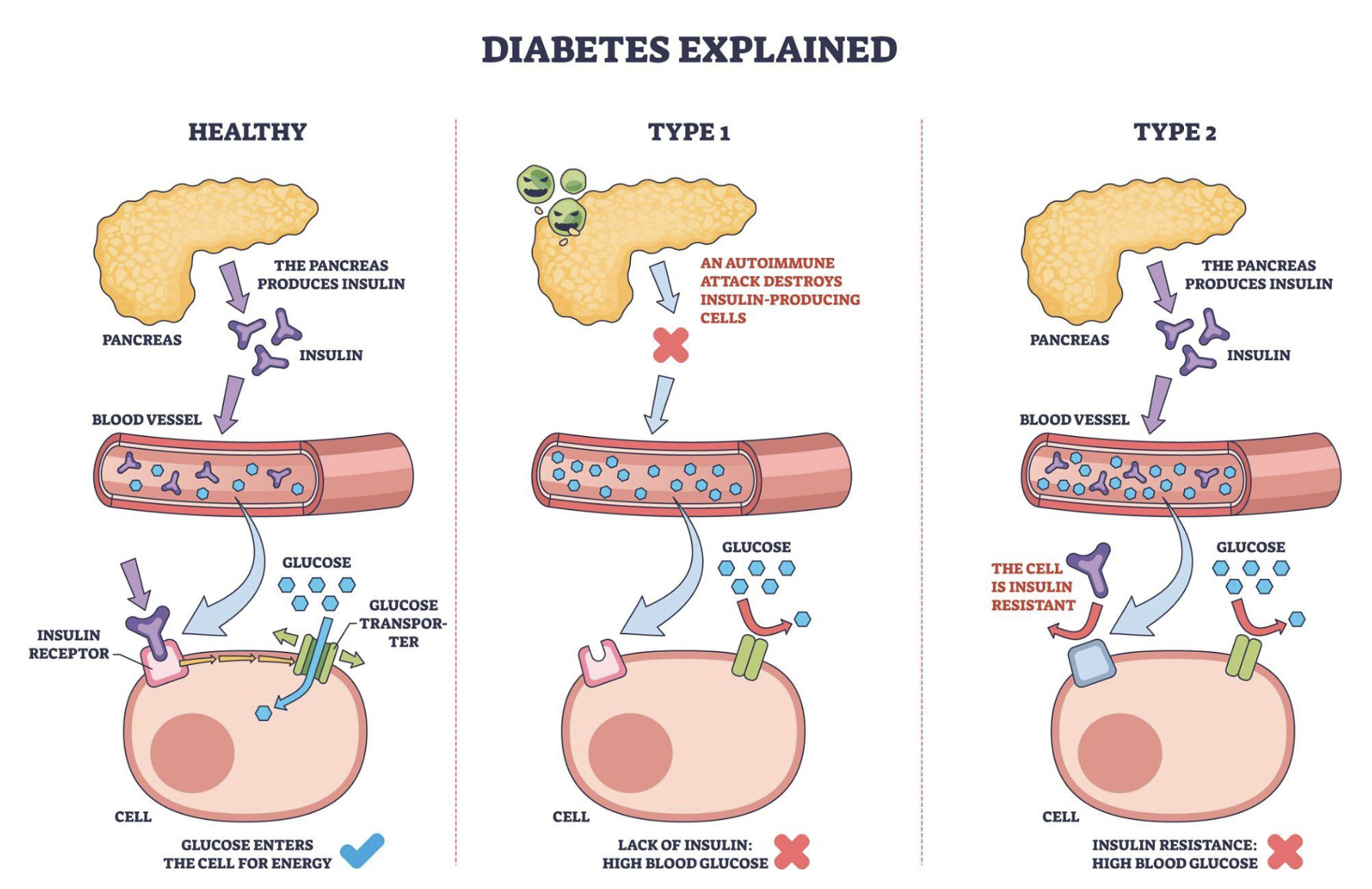
Type 2 diabetes is a chronic metabolic disorder characterized not by a single failure, but by a progressive breakdown of the body’s ability to regulate glucose, in which insulin—initially present and often elevated—gradually loses its effectiveness as a signaling hormone, leading to sustained hyperglycemia and a cascade of systemic consequences that extend far beyond blood sugar itself.
Unlike Type 1 diabetes, which emerges through autoimmune destruction of insulin-producing beta cells, Type 2 diabetes develops insidiously over time, often remaining clinically silent for years while underlying metabolic dysfunction advances, shaped by a complex interaction of genetic predisposition, environmental exposure, and behavioral patterns that accumulate rather than trigger abruptly.
What makes the condition particularly significant is not only its prevalence, but its nature as a systems-level disorder: it reflects a disruption in energy regulation, hormonal signaling, vascular integrity, and cellular responsiveness, positioning it less as an isolated disease and more as a long-term physiological imbalance.

How Type 2 diabetes affects the body
Under normal conditions, insulin functions as a regulatory interface between circulating glucose and cellular uptake, enabling tissues—particularly muscle and liver—to absorb glucose and convert it into usable energy or stored reserves.
In Type 2 diabetes, this regulatory system becomes impaired through a process known as insulin resistance, in which cells progressively lose sensitivity to insulin’s signal, forcing the pancreas to compensate by increasing insulin production in an attempt to maintain equilibrium.
Over time, three interconnected dynamics emerge:
cellular responsiveness declines, reducing glucose uptake efficiency
circulating glucose levels rise, creating a persistent hyperglycemic state
pancreatic beta cells become overburdened and gradually lose functional capacity
This triad results in chronic metabolic stress that affects multiple organ systems simultaneously, including vascular networks, neural pathways, renal filtration mechanisms, and ocular structures, explaining why diabetes is associated with complications that appear unrelated at first glance but share a common biochemical origin.
Common symptoms of Type 2 diabetes
One of the defining challenges of Type 2 diabetes lies in the subtlety of its early manifestations, as symptoms often develop gradually and may be misinterpreted as routine fatigue, aging, or lifestyle imbalance rather than indicators of an underlying metabolic shift.
The most frequently reported symptoms include:
increased thirst resulting from osmotic imbalance
frequent urination as the body attempts to eliminate excess glucose
persistent fatigue linked to inefficient cellular energy utilization
blurred vision caused by fluid shifts in ocular tissues
delayed wound healing due to impaired circulation and immune response
unexplained weight fluctuations reflecting metabolic instability
Because these symptoms rarely appear simultaneously or dramatically, many individuals remain undiagnosed until incidental testing reveals elevated glucose levels, at which point the condition may already be well established.
Early warning signs you should not ignore
Before classical symptoms become clinically evident, the body often presents a series of low-intensity signals that reflect early metabolic dysregulation, which are frequently dismissed due to their nonspecific nature.
These early indicators may include:
persistent low energy despite adequate rest
rapid fluctuations in energy levels following meals
increased hunger shortly after eating, suggesting impaired glucose utilization
cognitive fog or reduced concentration linked to unstable glucose supply
Individually, these signs may seem inconsequential; collectively, they form a pattern that suggests the body is struggling to maintain metabolic balance, making early recognition a critical factor in prevention and intervention.
What causes Type 2 diabetes
Type 2 diabetes does not arise from a singular cause but rather from the cumulative interaction of multiple risk factors that converge over time, gradually shifting the body from metabolic flexibility toward dysfunction.
Primary mechanisms:
Insulin resistance, which disrupts cellular glucose uptake
Genetic predisposition, influencing baseline metabolic sensitivity
Adipose tissue accumulation, particularly visceral fat that alters hormonal signaling
Sedentary behavior, reducing insulin efficiency
Dietary patterns high in refined carbohydrates and sugars, contributing to chronic glucose elevation
Additional contributing factors:
age-related metabolic decline
hypertension and cardiovascular stress
hormonal imbalances affecting glucose regulation
history of gestational diabetes
According to the World Health Organization, the global increase in Type 2 diabetes reflects not only individual behavior but broader structural changes, including urbanization, reduced physical activity, and shifts in dietary patterns, indicating that the condition is both biological and environmental in origin.
How Type 2 diabetes is diagnosed
Diagnosis relies on quantifiable biochemical markers that reflect both immediate and long-term glucose regulation, allowing clinicians to assess not only the presence of hyperglycemia but its persistence over time.
The primary diagnostic tools include:
fasting plasma glucose, measuring baseline blood sugar levels
HbA1c, indicating average glucose exposure over approximately three months
oral glucose tolerance testing, evaluating the body’s response to glucose intake
These measurements are interpreted within established clinical thresholds to distinguish between normal metabolic function, prediabetes, and confirmed diabetes, with guidelines from the Centers for Disease Control and Prevention emphasizing the importance of early detection, particularly in individuals with elevated risk profiles.
Treatment options and management
While Type 2 diabetes is classified as a chronic condition, its progression is highly responsive to intervention, and in certain cases, particularly in early stages, substantial metabolic improvement—or remission—can be achieved through sustained changes in behavior and physiology.
Lifestyle intervention as a foundation
Effective management begins with structural lifestyle adjustments:
dietary regulation focused on glycemic control rather than restriction alone
consistent physical activity to improve insulin sensitivity
weight reduction, particularly targeting visceral fat
Pharmacological support
When lifestyle measures are insufficient, medical therapy may be introduced:
metformin as a first-line agent improving insulin sensitivity
insulin therapy in advanced or uncontrolled cases
newer drug classes targeting glucose regulation pathways
Continuous monitoring
Long-term stability depends on ongoing assessment:
blood glucose tracking
evaluation of dietary responses
adjustment of physical activity patterns
The objective is not temporary correction but sustained metabolic equilibrium.
Living with Type 2 diabetes
Living with Type 2 diabetes involves a shift from reactive treatment to proactive management, where consistency replaces intensity and small, repeatable behaviors accumulate into measurable outcomes.
Individuals who maintain stable control typically adopt a structured yet flexible approach, integrating dietary awareness, regular movement, and continuous feedback from their own physiological responses, rather than relying solely on external interventions.
Over time, this adaptive process not only stabilizes glucose levels but reduces the likelihood of complications, reinforcing the principle that long-term outcomes are shaped by daily patterns rather than isolated decisions.
When to see a doctor
Medical evaluation should be sought when symptoms persist or patterns emerge that suggest underlying metabolic disruption, particularly in the presence of risk factors.
Key indicators include:
ongoing fatigue without clear cause
persistent thirst or increased urination
sudden visual disturbances
unexplained weight changes
Early diagnosis significantly alters prognosis, as intervention at an earlier stage can prevent or delay the progression of systemic damage.
Why understanding Type 2 diabetes matters
Type 2 diabetes represents more than a clinical diagnosis; it is a reflection of how the body responds to prolonged metabolic pressure, where imbalance accumulates gradually before becoming visible.
Understanding this process transforms the condition from an abstract label into a manageable system, where awareness enables intervention and consistent action reshapes trajectory.
The distinction between progression and control is rarely determined by a single factor, but by the alignment of knowledge, behavior, and timing.
FAQ
Can Type 2 diabetes be reversed
In early stages, significant lifestyle changes—particularly weight loss and dietary adjustment—can lead to remission, though ongoing management remains essential.
Is Type 2 diabetes genetic
Genetics influence susceptibility, but environmental and behavioral factors determine whether the condition develops.
Is it dangerous
Without management, it increases the risk of cardiovascular disease, nerve damage, kidney failure, and vision loss.
Do you always need insulin
No, many individuals manage the condition effectively through lifestyle and oral medications, depending on disease progression.
